The cornea is the transparent tissue comprising the anterior arched part of the eye, covering the iris. Various causes, infectious or not, can cause inflammations of the cornea.
The basic problem with inflammations of the cornea is that vascularization and scarring, occurring during tissue restoration phase, lead to loss of its transparency or creation of astigmatism resulting in serious decrease of the patient’s vision.
Herpes Keratitis
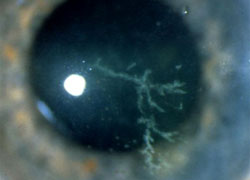 The typical appearance of herpes keratitis is characterized by the presence of a dendritic ulcer, an ulcer on the cornea surface with branches that resemble tree branches. In other cases, it can take the form of punctate keratitis with random small chalky foci. The sensitivity of the cornea is also characteristically reduced.
The typical appearance of herpes keratitis is characterized by the presence of a dendritic ulcer, an ulcer on the cornea surface with branches that resemble tree branches. In other cases, it can take the form of punctate keratitis with random small chalky foci. The sensitivity of the cornea is also characteristically reduced.
The first contact with the virus often occurs during childhood and is asymptomatic. The herpes virus can be permanently established at some nearby point of the nervous system and migrate to the eye and cause inflammation during periods when the body’s defense is weakened.
Herpes Keratitis often relapses. The repeated attacks create opacities in the cornea, which becomes like a geographical map.
The use of local steroids on an active herpes ulcer must be avoided, because it can deteriorate the disease and delay its healing. Herpes Keratitis is treated with antiviral agents, such as acyclovir (Zovirax), administered, according to the case, as an ophthalmological ointment or/ and systematically with pills.
Adenovirus Keratitis
Although conjunctivitis is very frequent, the infection rarely spreads to the cornea.
Its clinical appearance is characterized by multiple whitish opacities, causing vision decrease. The treatment includes local steroids that must be used only when the possibility for herpes keratitis has been excluded.
Bacterial Keratitis
The epithelium, the outer cornea layer, constitutes an effective barrier, preventing the entrance of most pathogen microorganisms in the eye. However, a necessary condition to perform this function is its integrity. After an injury, prolonged xerophthalmia or other causes disturbing the integrity of the epithelium, microorganisms may invade the deeper corneal layers and cause a very serious inflammation.
The most common microbial causes are staphylococcus epidermidis and pneumococcus, while pseudomonas infection is an especially threatening condition, frequently associated with prolonged use of contact lenses. Contact lens users must be extremely cautious. Symptoms, such as discomfort, pain, redness, vision clouding, discharges etc., dictate a visit to the ophthalmologist for further examination.
The microbial infections and ulcers of the cornea are emergency conditions, for which hospitalization and intensive treatment are required.
Acanthamoeba Keratitis
Acanthamoeba is a pathogenic microorganism found in the soil, water, sewage systems, coolers and air conditioning systems, which can cause a serious corneal infection.
It poses a great threat for contact lens users, who do not observe hygiene rules when storing, using and disinfecting their lenses. Using tap water or infected solutions for cleaning lenses, swimming or bathing with contact lenses etc., predispose for the development of such an infection, which, albeit rare, is extremely serious.
Non response to usual antibiotics is a characteristic of the disease. Therefore, a visit to the ophthalmologist and the administration of appropriate treatment are imperative.
Fungal Keratitis
Fungal Keratitis of the cornea usually occurs after an injury involving plant material, such as tree branches, thorns etc.
Other predisposing factors are contact lenses (as fungi can multiply in the manufacturing material of soft lenses), immunosuppression due to drugs or disease, surgical procedures and abuse of anaesthetic eye drops.
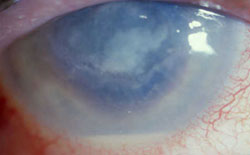 The symptoms start slowly with a feeling of foreign body, gradually increasing pain,, and redness, while clinically satellite lesions and hypopyon are often clinically present.
The symptoms start slowly with a feeling of foreign body, gradually increasing pain,, and redness, while clinically satellite lesions and hypopyon are often clinically present.
The treatment starts after the laboratory confirmation of the microorganism responsible and includes pharmaceutical and, in certain cases, surgical treatment.
Noninfectious Keratitis
An inflammation of the cornea can also develop as a result of noninfectious causes, such as various acquired or congenital dystrophies and degenerations of the cornea, neurotrophic causes, metabolic diseases, toxic agents, drugs etc.
All these conditions must be recognized and treated in time, because in many cases, the inflammatory reaction can cause irreversible damage on the cornea and the only solution to restore vision is transplantation (keratoplasty).
 German
German Ελληνικά
Ελληνικά